
Sleep – Awareness Week 2021
What is SUDI?
Recently I completed The National Sudden Unexpected Death in Infants (SUDI) online prevention program and it has got me thinking a lot about safe sleep. I know for me, pregnant with my first son Peter, SUDI or SIDS and “Cot Death” as it has previously been known; was one of my biggest fears. Luckily for me, Peter quite happily slept on his back, swaddled and in his own bassinet. But when Tobias came along he fought the swaddle and hated being on his back. In fact, he rarely slept unless perched over my shoulder like a drunk parrot. In those early days I didn’t know that he had Laryngopharyngeal reflux which was the cause of his discomfort and attributed to his struggle with sleep.
Sudden Unexpected Death in Infants (SUDI) is a term used to describe the sudden and unexpected death of a baby less than 1-year-old in which the cause was not obvious before investigation.
In the 1980’s SUDI rates were the highest in the world here in New Zealand. A 3 year “cot- death” study was done, which identified three modifiable risk factors:
- prone (on the tummy) sleep position,
- maternal smoking and
- lack of breastfeeding.
New Zealand led the way with a “Back to Sleep” campaign which saw mortality rates halve within just two years of its launch and it has since gone on to be implemented in most developed countries.
What have we learnt?
So what is the takeaway message from these studies and campaigns? In order to protect our tamariki we must remember PEPE:

P – Place baby in their own bed: Always place your baby in their own sleep space but close to their caregiver (this led to the introduction of pepi pods, see image). The space should have a firm, flat, well fitted clean mattress with light bedding to avoid overheating which cannot come over their head. The environment should be free of soft furnishings such as cot bumpers and soft toys.
E – Eliminate smoking during pregnancy: Make sure you protect your baby with a smoke-free family (whanau), home (whare) and car (waka). Babies born to smoking mothers have a reduced lung capacity due to their lower birth weight but they also have a defect in arousal which puts them at an increased risk of SUDI.
If you want support to give up smoking:
Call the Quitline on 0800 778 778 or text 4006 – it’s free
Check out the Quitline/Me Mutu website: https://quit.org.nz/en/reasons-to-quit/smoking-and-pregnancy?gclid=CjwKCAiAnfjyBRBxEiwA-EECLKE10A2au8ZwcLKs-rm1n97HTHK0aI0vKEp9SXaYeBlZparsE49_JBoCHQoQAvD_BwE
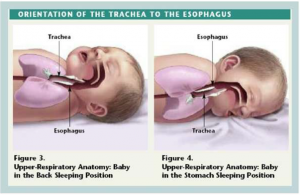
P – Position baby on their back to sleep: Studies show that babies may actually clear secretions better when placed on their backs. When a baby is in the back sleeping position the trachea lies on top of the oesophagus. Anything regurgitated or refluxed from the oesophagus must work against gravity to be aspirated into the trachea. Conversely, when a baby is in the stomach sleeping position, anything regurgitated or refluxed will pool at the opening of the trachea, making it easier for the baby to aspirate.
E – Encourage and support mum to breastfeed: Wherever possible breastfeeding should be initiated. Your breastmilk makes a huge difference to your baby’s health. Breastfed babies wake often to feed; this arousal is actually an inbuilt safety mechanism.
If you need support with breastfeeding contact your local La Leche leader: https://lalecheleague.org.nz/get-help/
What if I can’t breastfeed or choose to bottle feed?
If you are unable to breastfeed talk to your midwife, doctor or nurse first. The link below gives great advice from the Ministry of health around safe bottle feeding practices: https://www.healthed.govt.nz/resource/feeding-your-baby-infant-formula
The Nutricia Care line can put you in touch with a registered health care professional and can help you to decide which formula is best for your baby. Ph. 0800 438 500. You can also check out their website at: https://nutricia.co.nz/early-life-nutrition/aptamil
Can our babies sleep anywhere else safely?
A recent study showed that parents drive an average of over 1,500KM a year to give their little ones some shut eye! And yes, I am one of those parents! But is it safe? It is NOT safe to have your child sleeping in a car seat that is not in a moving vehicle. This is because the movement of the car stimulates breathing, so, once home you should then transfer them to a firm flat surface, or, just keep cruising until your little one wakes and enjoy the ride!
You may have heard about the Fisher Price Rock and Play recall, last year. This product was popular with parents because it was a bassinet type rocker on an incline. It was sold as a sleep product but it had absolutely no safety testing. Babies slept well in it but many babies also died as they were able to roll and suffocate. Babies should never be placed in rockers or bouncers for sleep.
For me, with Tobias especially, baby wearing has been a lifesaver. But even carriers and slings have risks and there have been deaths associated with suffocation so care must be taken. The adult using the carrier must make sure the babies nose and mouth are free at all times and that the airway is not occluded by a chin on the chest position. Care should be taken not to impair breathing or cause overheating by covering these carriers with a coat or blanket. One study recommends that soft carriers should not be used until the baby can hold his head up alone and contraindicates use prior to four months.
What about inclining the cot?
Many of us may also have been told to raise the cot head in order to reduce reflux symptoms but this is now changing too. Recent research has shown elevating the head of the cot does not clinically improve reflux symptoms. But it does pose an increased risk of SUDI as it may cause the baby to slide down to the foot of the cot into a position that could compromise breathing. Placing a pillow or wedge under the mattress or in the cot with the aim of elevating the baby’s head is also not recommended as it increases the likelihood of baby slipping down under the bedding and the baby’s head becoming covered.
Will our babies ever sleep?

I think sleep and babies has to be the biggest and most controversial subject in parenting. I have had complete strangers ask me if my baby sleeps through the night? What is our obsession with this? Peter is almost 2.5 years and rarely sleeps through the night. Tobias at 1-year-old still feeds A LOT at night, which is biologically normal for a baby of his age. Am I tired? Yes! So very tired some days! But I have learnt to accept that my boys will wake at night and given they both have respiratory issues, I choose to see this as a good thing. There is no magic answer when it comes to sleep, and reflux babies struggle all the more. What we can offer is support, understanding and compassion and that is what our community is all about. But what we must also remember is that we must place our babies in a safe place to sleep every sleep because the price we could pay for not, is too high to speak of.
Written by Jenny Overwater, National Coordinator and Mum of two amazing boys for March 2020 Newsletter.
Resources/ Related links:
- http://sudinationalcoordination.co.nz/sites/default/files/2017-09/otalaryngological.pdf
- https://pediatrics.aappublications.org/content/pediatrics/early/2011/10/12/peds.2011-2284.full.pdf?fbclid=IwAR2cw4AoYXeapHYFRQ7ZGDv-6Y70YURSyMUBsFgo3LdEiNlpNFkBHAByFWs
- https://www.plunket.org.nz/caring-for-your-child/safe-sleep/safe-co-sleeping/#using-a-pepi-pod
- https://www.kidshealth.org.nz/safe-sleep-your-baby)
- https://babyology.com.au/parenting/family/study-finds-desperate-parents-drive-1500-km-per-year-putting-kids-to-sleep/?fbclid=IwAR1xDRGiTlwQtfgVCfxlVpc24jJ2rzBXaXu_SjWnvdTnDLSbW3oZOju3mMg
- https://www.washingtonpost.com/business/economy/how-fisher-price-invented-a-popular-baby-sleeper-without-safety-tests-and-kept-it-on-the-market-even-as-babies-died/2019/05/30/78c2707a-7731-11e9-b3f5-5673edf2d127_story.html?arc404=true
- https://www.researchgate.net/publication/280123964_Sudden_deaths_in_adult-worn_baby_carriers_19_cases
- https://rednose.org.au/article/sleeping-position-for-babies-with-gastro-oesophageal-reflux-gor
© Crying Over Spilt Milk Gastric Reflux Support Network New Zealand May 2021.




